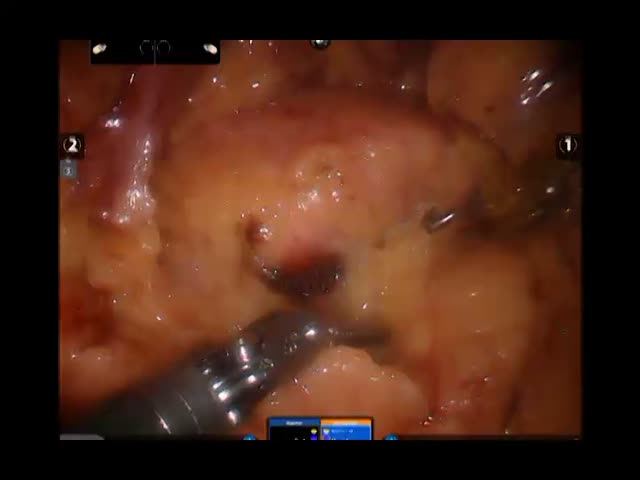
Robotic Whipple, Pylorus Preserving Pancreaticoduodenectomy with Pancreaticogastrostomy
April 28, 2012
Pier C. Giulianotti (Chicago – USA) Francesco Bianco ( Chicago – USA) Luca Milone (New York – USA)
Previous Surgeries: Cholecystectomy and appendectomy.
Histology: Intraductal papillary mucinous neoplasm, Tumor size: 1.5 x 1.0 x 1.0 cm, Margins of resection are free of tumor, the closest esection margin (anterior) is 1.0 cm from the lesion. Pancreatic intraepithelial neoplasia (PANIN), grade 2/3. Margins of resection are free of PANIN.
History: a past medical history significant for recurrent episodes of pancreatitis and presence of pancreatic cyst
Surgery Description: The patient has been diagnosed with a cystic lesion in the head of the pancreas and one of the differential diagnosis of benign mucinous cyst or mucinous dysplasia of the ducts and for the risk of developing cancer. Finally the resection of the head of the pancreas has been considered. A minimally invasive approach has been offered and after consent has been obtained the procedure was planned.
Ports: Introduction of a 5-mm port in the left upper quadrant and preliminary exploration of the abdominal cavity. There are a few omental adhesions in the upper quadrant. Another 5-mm trocar close to the umbilicus and more trocars are placed to complete the procedure. Two 10 mm trocars placed on both sides of the umbilicus, two 8 mm size trocar laterally in the right upper quadrant, one 8 mm size in the left upper quadrant.
Steps:
1 – Dissection of the right colonic flexure from the liver. The flexure is mobilizes and the second portion of the duodenum identified in the Kocher maneuver with mobilization of the head of the pancreas and the descending portion of the duodenum. Cava and the aortocaval space are exposed.
2 – Dissection of gastrocolic ligament using the harmonic device. The lower border of the pancreas is exposed.
3 – After exposing the neck of the pancreas and the confluence of the superior mesenteric vein with the portal vein, we are working at the hilum of the liver taking down some adhesions, exposing the common bile duct. Using the fluorescence we are able to confirm the anatomy of the bile duct, the
bifurcation and to follow the bile duct distally: note the anatomy of the hepatic artery that has a normal bifurcation with the right branch posterior to the bile duct. Transection of the right gastric artery in between sutures and of the common bile duct.
4 – The common hepatic artery is prepared until reaching the celiac artery. After the transection of the gastroduodenal artery, we are exposing the portal vein and the superior edge of the neck of the pancreas.
5 – Then the first portion of the duodenum is transected. The following step is to go to the Treitz and transecting the first jejunal loop in between the stapler device and retracting the duodenojejunal flexure on the right side posterior to the superior mesenteric vessel. Two stitches of Prolene 3-0 are applied on the neck of the pancreas and using Harmonic device, the neck of the pancreas is transected.
6 – Dissection of the uncinate process. The superior mesenteric vein is prepared on a vessel loop. We are exposing the SMA and removing all the lymphatic tissue between the SMV and the SMA.
7 – Completion of a radical pancreaticoduodenectomy Whipple type with the preservation of the pylorus. Momentarily the specimen is left inside the abdominal cavity and we are starting the immediate reconstruction.
8 – The pancreatic duct is small in size and a small stent is placed inside the pancreatic duct. A Gastrostomy is performed. Interestingly, stomach shows presence of multiple polyps that are biopsied and sent to permanent pathology. Then the first jejunal loop is brought retromesenterically up to the liver and an anastomosis between the bile duct and the jejunal loop and hepaticojejunostomy end-to-side are performed. using PDS 5-0. The last reconstruction in between the stomach, the pylorus and the jejunum is performed using the same jejunal loop 40 cm distal to the hepaticojejunostomy.
The patient has been stable for the entire procedure. Overall blood loss between 250 and 300
cc of blood, not requiring an intraoperative transfusion.